THE BASICS
Chronic inflammation occurs later on in the inflammatory process following the initial cleanup attempt by the acute inflammatory process. It occurs when tissue injury and repair attempts overlap.
The key inflammatory cells in chronic inflammation = Mononuclear cells: Macrophages + lymphocytes) (Remember acute inflammation = neutrophils ).
Chronic inflammation can occur as the result of:
Persistence of infection or foreign body not resolved with acute inflammation
Toxic agents (prolonged, continued exposure)
Atherosclerosis = the deposition and accumulation of cells and extracellular materials in vascular walls. MECHANISM OF ACTION= Monocytes in the blood stream can pass through the epithelium where they become caught in the intima --> differentiate into macrophages --> promote inflammatory responses. --> Cells, lipids, and collagenous materials accumulate --> form atherosclerotic plaque --> if a plaque continues to grow large enough, it can causbe blood flow obstruction, can rupture & trigger the inflammatory respose, or it break free and embolize to a distant site (+/- causing obstruction there).
Hypersensitivity reactions: Classic example is asthma- associated with inc eosinophils (instead of the usual inflammatory cell of chronic inflammation- macrophages). Eos release a highly toxic substance called major basic protein, and lipid bodies that enhance eicosanoid production. The result= chronic inflammation and bronchial wall remodeling causing narrowing of the airways.
MACROPHAGES IN CHRONIC INFLAMMATION
Because macrophages are the primary player in chronic inflammation, we'll focus on them. However, be aware that neutrophils, can be still be found at sites of chronic inflammation. This is sometimes referred to as "acute on chronic inflammation", or "chronic active inflammation".
Macrophages = tissue version of monocytes (Recall monocytes arise from the bone marrow (adults) or yolk sac/liver (fetus) . They then enter the bloodstream where they are called monocytes. Once they leave the bloodstream and enter the tissues, they are now considered "macrophages" which can become activated where they will now be referred to as "histiocytes")
Macrophages/histiocytes can go by different names depending on what tissue they ended up in:
Liver = Kupffer cells
Spleen and lymph nodes = Sinus histiocytes
Central nervous system = Microglial cells
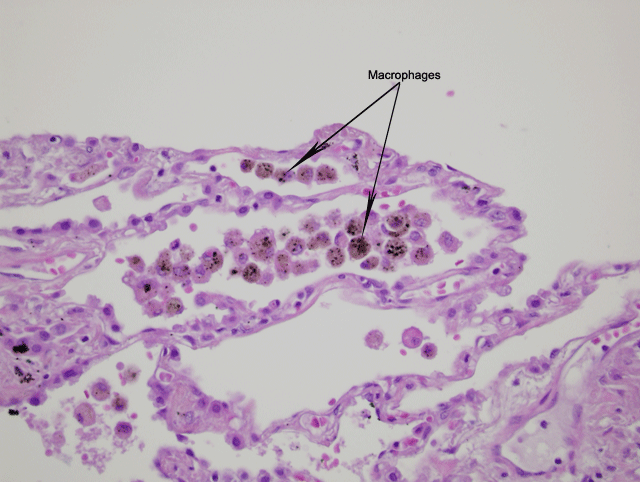
Lung alveoli = "Hemosiderin-laden" macrophages, "Heart-failure cells" or "anthracotic pigmented histiocytes"
Macrophage Activation
Initial Stimulus
Microbes
Interferon gamma (IFN-gamma, aka type II interferon) is a cytokine produced by activated T cells (note this is a part of a positive-feedback loop)
Pro Inflammatory Effects:
Activated macrophages will continue the inflammatory response by:
Producing inflammatory cytokines, chemokines, & antimicrobial products to call in more inflammatory cells to the site of inflammation (Ex: inducible nitric oxide, reactive oxygen species, and lysosomal enzymes, tumor necrosis factor). These help.
Serving as antigen presenting cells/APCs to activate T cells- basically the macrophage presents the "junk" at the site so the lymphocytes know what is "bad" and can start their "search & destroy" mission
Anti-inflammatory effects:
T cells release anti-inflammatory cytokines (Interleukins 13 and 4 (IL-13, IL-4).Interleukins 13 and 4 (IL-13 and IL-4) once all is resolved to tell the macrophage, "it's time to switch your mission plan and stop further inflammation/damage to the tissue". In response, macrophages produce:
Interleukin-10 (IL-10) to prevent excessive inflammation and damage to host cells.- > It will stop pro-inflammatory T cells, NK cells, and other activated macrophages
Growth factors that promote tissue repair- Ex: Vascular endothelial growth factor (VEGF), to build new blood vessels (promote angiogenesis), and transforming growth factor beta (TGF-ß), which facilitates deposition of extracellular matrix proteins for fibrosis.
POSSIBLE "END RESULT" OF CHRONIC INFLAMMATION
1. Complete resolution of the infection/foreign body reaction with limited damage to the host
2. Persistent infection +/- Granuloma formation- occurs when early anti-inflammatory immune responses are unable to eradicate the pathogens.
Tuberculosis is a classic example of a disease in which the infectious agent (Myocbacterium tuberculosis) persists via the formation of granulomas (organized collections of differentiated macrophages and lymphocytes that form around the bacteria to "wall it off" to prevent it from spreading). The granulomas of tuberculosis are characterized by caseous necrotic centers ("caseous" means they have a cheese-like appearance). NOTE: Some people think granulomas can actually facilitate the spread of bacteria as necrotic macrophages release their bacterial contents, new macrophages may engulf them and carry them to new sites.
Macrophages can have a wide variety of appearances in granulomas:
Multinucleated "giant cells": macrophages that have merged together become these multinucleated "giant cells", often at the periphery
Epithelioid cells- have interdigitating cell membranes,
Foam cells, - contain lipids.
3. Fibrosis/Scarring of tissue resulting in tissue loss & may cause end organ failure
Fibrosis is characterized by excessive collagen deposition in response to persistent stimulation; it results in tissue loss and organ failure.
Examples of excessive organ fibrosis include:
Liver cirrhosis
Constrictive pericarditis
Scleroderma
Lung fibrosis disorders (interstitial lung disease/ alpha 1 antitrypsin deficiency)
References
These notes were adapted and modified from the awesome medical education website, DrawItToKnowIt.com. This is a GREAT website for visual learners. Please subscribe to their website to view the complete lecture and see step by step drawings and charts.
Use coupon code ZXG2DM8ZJ to get 15% off your DrawItToKnowIt.com subscription.
Click HERE to subscribe (link opens in new tab).
Reference: Drawittoknowit.com "Chronic Inflammation" lecture. Accessed 3/21/19.
Klatt, Edward C. "Robbins and Cotran Atlas of Pathology". Chapters 1-4. 3rd ed. 2015.